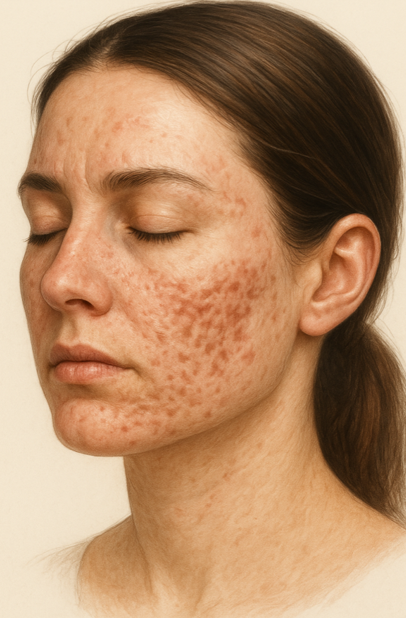
Acne is a multifactorial pathology of the pilosebaceous unit that affects 90% of adolescents but can also affect women between 30 and 55 years of age (so-called late acne).
Its etiopathogenesis involves an increase in Cutibacterium acnes (formerly called Propionibacterium acnes), an inflammatory process, and hormonal imbalances. Studies indicate that a diet with a high glycemic load and rich in dairy products, especially skimmed milk, is detrimental.
The European and American guides establish the medical treatments that should ideally be prescribed by dermatology specialists: these include topical and oral antibiotics (no more than 3 consecutive months), topical treatments with benzoyl peroxide, vitamin A derivatives (adapalene), 5% dapsone, hormonal treatment with oral contraceptives, metformin and spironolactone in cases of polycystic ovaries and in severe cases of nodular acne isotretinoin (which can be given at low doses but never intermittently). It is often useful to supplementation with Zinc, omega 3 and omega 6, equol, sulfophanes from broccoli and probiotics.
Studies show that several effective complementary treatments exist for the comprehensive management of active acne, but in all cases, they must be used in conjunction with the dermatological treatment indicated for each individual case. These include chemical peels, low-intensity light therapy, photodynamic therapy, and laser treatments.
Chemical peels: Evidence in the literature indicates that chemical peels are useful, especially when combined with individualized medical treatment, for the treatment of mild to moderate acne. The most effective substance is salicylic acid , which can be used in concentrations of up to 30%. It has keratolytic effects, unclogging sebaceous glands, as well as anti-inflammatory and bactericidal effects against Propionibacterium acnes 3, the strain found in high concentrations associated with acne.
Low-intensity light therapy: It uses light-emitting diodes (LEDs) at low energy densities (less than 5 J/cm²). Its mechanism of action is at the cellular level (cell membranes, mitochondria, and nucleus), regulating cellular functions. Unlike destructive laser therapies, there is no pain or heat. For acne, we will use two colors: red light due to its anti-inflammatory properties and the blue light due to its bactericidal action against Cutibacterium acnes. It is a treatment that can be combined with chemical peels and laser treatments to reduce their side effects.
Photodynamic Therapy (PDT): It uses LEDs, but first a photosensitizer is applied to the area to be treated. In these cases, pain, erythema, edema, and crusting will occur. Studies in the literature show that these treatments have shorter incubation periods and different sensitizers to try to reduce these side effects, and they demonstrate effectiveness in treating moderate to severe acne.
Laser Treatments: Laser treatments, especially pulsed dye lasers, have been used to treat acne. These treatments are based on destructive techniques targeting the sebaceous glands, resulting in heat and pain. Currently, photodynamic therapy (PDT) and lasers are not commonly used to treat active acne due to their adverse effects.
The current trend is to use treatments with an anti-inflammatory effect (non-aggressive chemical peels accompanied by low-intensity light therapy) since the primary role of inflammation in the pathogenesis of acne is being recognized.
The acne scars appear after suffering from inflammatory acne. Therefore, it is extremely important to treat acne to prevent these unsightly scars from forming. Acne scars are divided into atrophic and hypertrophic types. In this presentation, we will discuss the treatment of atrophic acne scars, which are the most common.
Atrophic scars are classified into three types, according to their morphology and depth: ice-beak, wavy, and punched. Often, these three types of scars coexist in the same patient. For ice-beak scars, the CROSS technique is the preferred method in most cases. (CHEMICAL RECONSTRUCTION OF SKIN SCARS).
THE SCAR SUBCISESION is the technique we most frequently use to treat acne scars and is the preferred method for wavy and pitted scars, especially when they vary in depth. Acne scars form as a result of the inflammatory process caused by acne. When this inflammation heals, fibrin tracts are created that pull the skin downwards, creating the depression of the atrophic scar. There is also a disruption of the epidermis, which loses its normal characteristics and takes on those of the scar. To allow the scar to rise, the first step is to break down these fibrin tracts using the subcision technique.
A small amount of hyaluronic acid is then injected into the base. This hyaluronic acid does not act as a filler; rather, by occupying space and pressing on the surrounding fibroblasts, it stimulates them to produce new collagen.
In a third step to improve the epidermis, improve hemostasis and for its bactericidal effect and to stimulate collagen synthesis, a CHEMICAL PEEL is carried out with salicylic acid and retinol.
Next, LOW INTENSITY LIGHT THERAPY will be applied due to its anti-inflammatory effects and its ability to stimulate collagen synthesis by fibroblasts.
There are recent publications on NEEDLING and PLATELET-RICH PLASMA (PRP), which may be helpful in some cases of superficial acne scars. RADIOFRECUENCY and different types of LASER have also proven useful in treating acne scars, but for the best results, COMBINED TECHNIQUES and individualized treatment of each scar will be key.